

Videos
 Video
Video
Converting Biologic Mesh to Synthetic, Absorbable Mesh
Vizient Mesh Savings Opportunity Podcast. Clinical benefits and savings opportunity
 Video
Video
Laparoscopic Ventral Hernia Repair using GORE® SYNECOR® BioMaterial
Carl R. Doerhoff, MD, FACS, practices in SurgiCare in Jefferson City, Missouri, presents the use of the GORE® SYNECOR® BioMaterial Laparoscopic ventral hernia repair.
 Video
Video
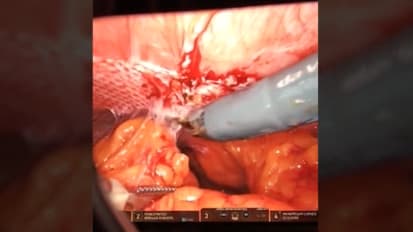
Robotic Sugarbaker Repair of a Parastomal Hernia utilizing GORE® SYNECOR Intraperitoneal Biomaterial
Karl A. LeBlanc, MD, MBA, FACS, FASMBS performs a Sugarbaker Repair of a Parastomal Hernia Utilizing GORE® SYNECOR Intraperitoneal Biomaterial 15 cm x 20 cm Synthetic Hybrid Mesh.
 Video
Video
This retrospective, multicenter, case review analyzed device/procedure endpoints and patient-reported outcomes in patients treated for hernia repair 1 year or more from study enrollment.
 Video
Video
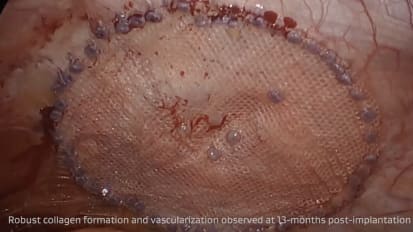
Post-Operative View: 13 Months Post Implantation
GORE® SYNECOR Intraperitoneal Biomaterial Lap ventral hernia repairs
 Video
Video
John Scott, MD, FACS, provides a post-operative clinical review of patients' quality of life after a hernia repair.
 Video
Video
Razvan Opreanu, MD, shares an 18-month post operative view using GORE® SYNECOR Intraperitoneal Biomaterial hybrid mesh.
 Video
Video
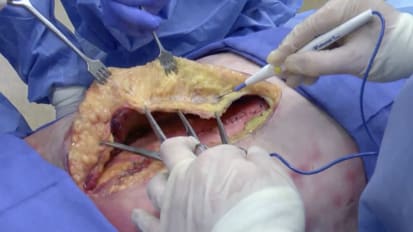
Posterior sheath mobilization in preparation for retromuscular hernia repair
John P. Fischer, M.D., MPH, FACS, is a specialist in abdominal wall reconstruction. This is a surgical technique video demonstrating the posterior sheath mobilization and creation of the retromuscular space.
 Video
Video
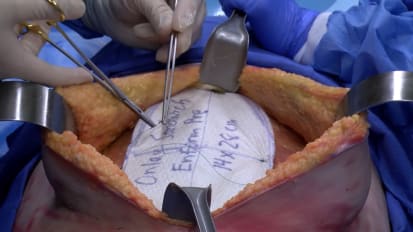
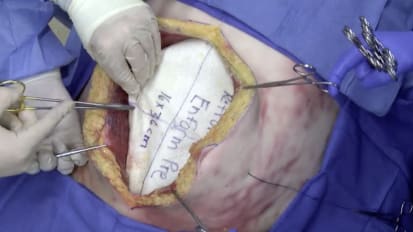
Retromuscular Onlay Hernia Repair Using GORE® ENFORM Preperitoneal Biomaterial
This is an educational surgical technique video demonstrating a retromuscular onlay hernia repair using GORE® ENFORM Preperitoneal Biomaterial. A cadaver model is used for demonstration to facilitate visualization of the anatomy. This ...
 Video
Video
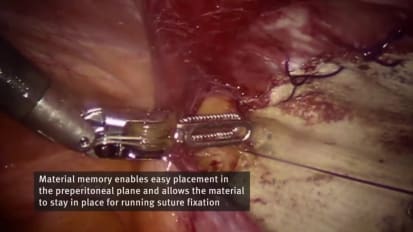
Robotic Preperitoneal Umbilical Hernia Repair
Robotic preperitoneal repair of an umbilical hernia utilizing GORE® SYNECOR Preperitonal Biomaterial by Matthew R. Reynolds, D.O.
 Video
Video
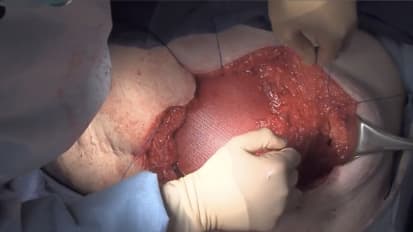
Ventral Hernia Repair Using the Components Separation Technique
Brent Mathews, M.D., FACS, performs a ventral hernia repair using the components separation technique.
 Video
Video
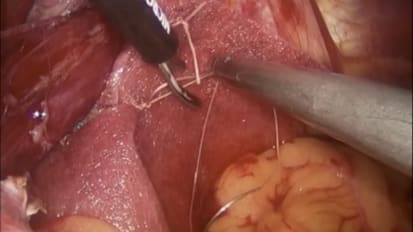
Paraesophageal Hernia Repair Using GORE BIO-A Tissue Reinforcement
William S. Cobb, IV, M.D., FACS, shares a video showing paraesophageal hernia repair using GORE BIO-A tissue reinforcement.
 Video
Video
Laparoscopic Fixation of GORE® SYNECOR Biomaterial in a Cadaver Model Using a Robotic Arm
Erik B. Wilson M.D., FACS, shares a video showing laparoscopic fixation of GORE® SYNECOR Biomaterial in a cadaver model using a robotic arm.
 Video
Video
GORE® BIO-A® Web Technology Innovation
Learn more about the GORE® BIO-A® Web Technology, and how it works as a scaffolding to help the body grow vascularized soft tissue.
 Video
Video
John P. Fischer, M.D., MPH, FACS, is a specialist in abdominal wall reconstruction. This is a surgical technique video demonstrating the retromuscular repair using GORE® SYNECOR Preperitoneal Biomaterial with transfascial fixation.
 Video
Video
John P. Fischer, M.D., MPH, FACS, is a specialist in abdominal wall reconstruction. This is a surgical technique video demonstrating retromuscular repair using GORE® ENFORM Preperitoneal Biomaterial with percutaneous fixation.
 Video
Video
Clinical Experience with GORE® SYNECOR Intraperitoneal Biomaterial
Donald Cugini M.D., presents a case using GORE® SYNECOR Intraperitoneal Biomaterial for umbilical hernia repair.
![Retromuscular Hernia Repair Using GORE<sup>®</sup> SYNECOR Preperitoneal Biomaterial with Transfascial Suture Fixation [Full Version]](http://res.cloudinary.com/broadcastmed/image/fetch/q_auto,c_fill,w_413,h_232,g_faces:center,f_auto/http%3A%2F%2F55933%2Dbcmed%2Es3%2Eamazonaws%2Ecom%2Fbcp%2Fimages%2ForlVideoAssets%2FimgSource%2Fwlg%5F0024%2Epng) Video
Video
John P. Fischer, M.D., MPH, FACS, is a specialist in abdominal wall reconstruction. This is a surgical technique video demonstrating a retromuscular repair using GORE® SYNECOR Preperitoneal Biomaterial with transfascial fixation.
 Video
Video
Trends, Tools, Trials: Complex Abdominal Wall Repair in 2020
Matthew I. Goldblatt, M.D., FACS, discusses a case study of a patient undergoing treatment for simultaneous colon and rectal cancers and had a prior low anterior colon resection procedure with a diverting ileostomy.
Documents
 Document
Document
Bio-A Mesh Use in Hiatal Hernia Repair. A Systematic Literature Review
Abdul-Rahman F. Diab, Joseph A. Sujka, Adham R. Saad, Christopher G. DuCoin, Salvatore Docimo present on hiatal hernia repair without mesh reinforcement that is associated with high rates of hernia reoccurrence, reaching more than 50% at 5 years.
 Document
Document
Long-term Outcome of Absorbable Synthetic Mesh in Clean Ventral Hernia Repairs
The use of absorbable synthetic mesh in clean wound ventral hernia repair resulted in favorable long-term recurrence rates.
 Document
Document
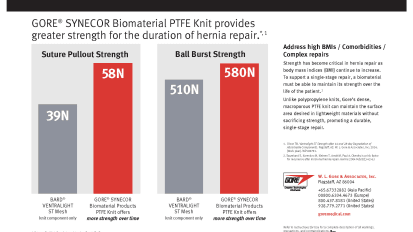
28-Day Strength Charts: GORE® SYNECOR Intraperitoneal Biomaterial
GORE® SYNECOR Biomaterial PTFE Knit provides greater strength for the duration of hernia repair.
 Document
Document
In early 2021, as part of the Gore Medical Mastery Series, a faculty of surgeons convened in a virtual hybrid symposium in the midst of the COVID-19 pandemic to discuss their approaches to AWR, hernia repair, and tissue reinforcement.
 Document
Document
GORE® BIO-A® Tissue Reinforcement offers proven low complication rates in high risk AWR patients1 vs. BARD® DAVOL PHASIX Mesh.
 Document
Document
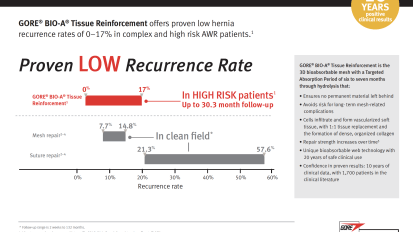
GORE® BIO-A® Tissue Reinforcement offers proven low hernia recurrence rates of 0–17% in complex and high risk AWR patients.
 Document
Document
Better AWR Outcomes. Reinforced by Data. Critical healing period and repair strength
GORE® BIO-A® Tissue Reinforcement provides a unique 3D tissue-building scaffold that elicits a specific tissue response during the critical wound healing period.
 Document
Document
GORE® BIO-A® Tissue Reinforcement is designed as an alternative to longer-term resorbable and permanent meshes to offer a strong repair while avoiding risk for long-term mesh-related complications
 Document
Document
Bioabsorbable Mesh for Hernia Repair: Know your Options
GORE® BIO-A® Tissue Reinforcement is intended for use in the reinforcement of soft tissue. GORE® BIO-A® Tissue Reinforcement may be used include hernia repair as suture-line reinforcement, muscle flap reinforcement, and general tissue reconstructions.
 Document
Document
Retro-rectus Placement of Bio-absorbable Mesh Improves Patient Outcomes
Our primary objective was to determine the longterm surgical outcomes of retro-rectus and intraperiteonal placement of mesh.
 Document
Document
This retrospective, multicenter, case review analyzed device/procedure endpoints and patient-reported outcomes in patients treated for hernia repair 1 year or more from study enrollment.
 Document
Document
A Patient’s Guide to Hernia Repair
While some hernia defects can disappear if they are pressed, this does not permanently resolve the hernia. In addition, because hernias typically worsen over time, the patient should consult a surgeon after a hernia has been identified.
 Document
Document
Visible tissue responsiveness: Metabolic and fibroblast activity during utilization of a bioabsorbable matrix in abdominal wall reconstruction
 Document
Document
In this issue of General Surgery News Special Report, Eric Mallico, M.D., FACS, describes the quality of life of patients after ventral and hiatal hernia repairs, and reviews long-term patient outcomes.
 Document
Document
A fundamental goal of hernia repair is providing a durable closure.
 Document
Document
The influx of more high-risk and obese patients in need of abdominal wall hernia repair naturally leads to larger, more complex hernia cases and the need for strong mesh.
 Document
Document
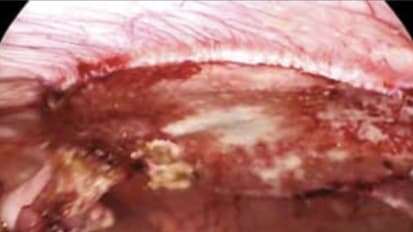
GORE® ENFORM Biomaterial is a reinforcement for soft tissue composed of synthetic bioabsorbable polyglycolic acid and trimethylene carbonate which has proven to be effective for hernia repair.
 Document
Document
Mesh Selection for Hernia Repair: Expert Review of Biologic, Synthetic and Bioabsorbable Types
Today, mesh closure is the standard in hernia repair, a credit to advances in materials and surgical techniques since usher.
 Document
Document
Learn More About GORE® SYNECOR Biomaterials
Hybrid hernia repair device for high BMIs, multiple comorbidities and recurrent defects are now available.
 Document
Document
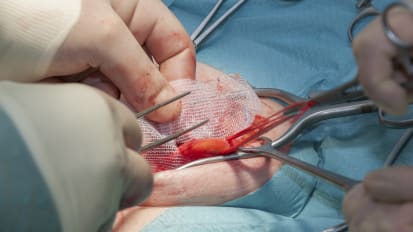
Expert Review: Clinical experience with GORE® SYNECOR Intraperitoneal Biomaterial
A surgeon reviewing their clinical experience with GORE® SYNECOR Intraperitoneal Biomaterial and MEDTRONIC PARIETEX Composite Mesh for Umbilical / Epigastric Hernias.
 Document
Document
Biosynthetics — Know your options
"[Biologic] materials come with only moderate durability, and at substantial financial cost. Slowly absorbable biosynthetic implants, as a class of hernia meshes, represent a possible cost-effective solution. In the final analysis."
 Document
Document
Many repaired incisional or ventral hernias recur; thus, the primary objective of research and technological developments pertaining to these hernias has long been to minimize recurrences without increasing treatment-related complications.
 Document
Document
Case Study: Proven Outcomes Reduced Costs for Complex Hernia Repairs
GORE® BIO-A® Tissue Reinforcement is an excellent choice in soft tissue repair, including complex hernia.
 Document
Document
A Cost Comparison of Mesh Usage in Laparoscopic Paraesophageal Hernia Repair
The aim of this study was to compare costs of the GORE® BIO-A® Device, ALLERGAN ALLODERM Device, and ALLERGAN STRATTICE Device in relation to the outcomes in terms of length of stay and recurrence rate following PEH repair.
 Document
Document
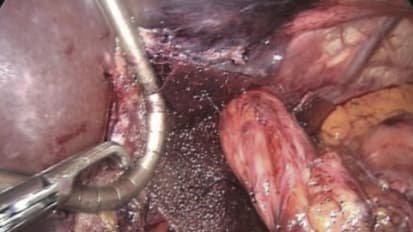
Biosynthetic Tissue Scaffold Recruits Progenitor Cells in Muscle Tissue Healing Model
This study demonstrates that the open, porous structure of the GORE® BIO-A® Tissue Reinforcement is able to recruit the Pax7+ cells residing in host muscle, a critical step in muscle regeneration.
 Document
Document
GORE® BIO-A® Tissue Reinforcement is a three dimensional resorbable mesh which has demonstrated to be a ideal “scaffold” facilitating tissue generation and healing without the risk of a non-resorbable implant.